By Jimmy Dale Smith, PT, DPT, The Healthcare Resort of Plano, TX
Myofascial decompression (MFD), or cupping, is a form of IASTM (Instrument Aided Soft Tissue Manipulation), where a pump and a cup are used to create negative pressure and placed on the skin to improve circulation/blood flow, reduce pain, improve tissue pliability/mobility and to improve healing.
Additional benefits of cupping may include improved quality/quantity or ROM, improved tolerance to ROM/PROM exercises, and excellent neural input to improve motor output. Contraindications include open wounds, fever/active infection, severe disease (cardiac, renal failure, bleeding disorder, hemophilia, active cancer and dermatitis), first trimester of pregnancy, unhealed or possible fracture, severe strain/sprain, or already inflamed/swollen tissue, burns and acute flare-ups of skin disease (psoriasis, eczema or rosacea).
- When: Depends; early in POC to assess patient’s response
- Where: Location of pain/perceived stiffness, myofascial line, neurovascular junction
- Why: ROM, pain, blood flow, soft tissue adhesions
- Who: Patients who do not have contraindications
- What: Reassess, test and retest
Pilot Study: Plano Health Care Resort
The Physical Therapy department at Plano HCR is currently one of our affiliates in Keystone that is piloting usage of cupping across patients with differing diagnoses, which has resulted thus far in varying degrees of success. Predominantly, the facility has observed a positive response to MFD. Through the observations, benefits range from an hour (to the end of the session) up to five to seven days of pain relief. One specific “home run” of treatments is the following case study.
Case Study: Mr. T.
Mr. T. is a mid-70s male s/p R TKA. He presented to PT as an outpatient seeking further rehab after his SNF stay.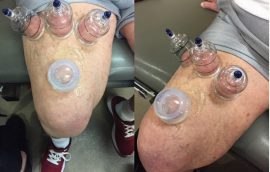 His primary limiting impairments were stiffness, pain and weakness. When he initially attempted basic OKC (open kinetic chain) activities, the patient would report moderate to severe pain at end-range knee extension. The team attempted to modify to a CKC (closed kinetic chain) to assess differences in symptoms. Stiffness remained. Moving to manual therapy, the patient responded decently well with anterior tibiofemoral mobilizations. The patient reported less pain, but the stiffness remained. The PT team applied three hard plastic cups with 1.5 pumps of pressure proximal to the knee as a gross stabilization point for the fascial system and one silicone cup just distal to those cups with the intent to perform a dynamic mobilization technique. Post-treatment, the patient reported that not only was the pain nearly eliminated, but the stiffness was gone as well.
His primary limiting impairments were stiffness, pain and weakness. When he initially attempted basic OKC (open kinetic chain) activities, the patient would report moderate to severe pain at end-range knee extension. The team attempted to modify to a CKC (closed kinetic chain) to assess differences in symptoms. Stiffness remained. Moving to manual therapy, the patient responded decently well with anterior tibiofemoral mobilizations. The patient reported less pain, but the stiffness remained. The PT team applied three hard plastic cups with 1.5 pumps of pressure proximal to the knee as a gross stabilization point for the fascial system and one silicone cup just distal to those cups with the intent to perform a dynamic mobilization technique. Post-treatment, the patient reported that not only was the pain nearly eliminated, but the stiffness was gone as well.
