By Elyse Matson, MA CCC-SLP, SLP Resource
The Free Water Protocol is one option SLPs may utilize to help counteract the adverse effects of thickened liquids and/or tube feedings. What is it? How should it be used in your facilities? What are the risks for aspiration pneumonia?
The (Frazier) Free Water Protocol was named after Frazier Hospital. In 1984, Frazier Hospital began to give all patients unlimited bedside water and/or ice chips. They found that fewer residents had UTIs and dehydration. They also found that when paired with proper positioning and oral care, there were no incidents of aspiration. Although it has been referred to as the “Frazier Water Protocol” in the past, the proper name is “The Free Water Protocol.” It is best used with patients on thickened liquids or patients who are NPO and on tube feeding.
The free water protocol is not appropriate for all patients. The below table can be used by the SLP to help determine the risk for pneumonia in each patient. As you might imagine, the higher the clinical complexity of the patient, the less likely a Free Water Protocol should be implemented. Remember that a patient on ice chips or free water has not been deemed free of aspiration on these textures; rather a determination is made that the benefits of free water outweigh the risk of pneumonia.
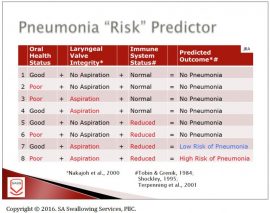
The Water Protocol is generally defined by these guidelines:
- Patient is allowed to drink water between meals (minimum of 30 minutes after meals)
- Water and ice chips cannot be provided during a meal if the resident is prescribed thickened liquids
- The prescribed thickened liquid is provided at meals
- Medication cannot be administered with water if resident is prescribed thickened liquids
- NPO patients can have water anytime
- Use all other swallowing guidelines
- Must abide by other fluid restriction orders
- Position upright always
- No thin water until oral care is completed or 30 minutes after meal
- Water is offered freely throughout the day
So what are the best methods to implement the Free Water Protocol? A multi-pronged approach is recommended.
First, a facility-wide training, including:
- Patient identification methods
- Facility-wide implementation as facility program not just a speech program
- Provision of oral care to patients at risk for aspiration
- Method for writing orders and care plan in PCC only after the oral care component is implemented
- Communication methods with Dietary, Nursing, MD and family
- Monitoring systems to assure the program is being followed
- Communication about the specific methods for each particular patient, including:
- Method for completing oral care
- Licensed or nurse aid providing oral care (check your state laws for who can use oral suction)
- If patient will receive unlimited or limited water or ice chips
- Swallow strategies required for best safety
- Documentation in place that states risks and benefits
- Clarity on who will monitor proper administration of the protocol
In some facilities, especially when first implementing the Water Protocol, the clinical team may prefer a doctor’s order that does not refer to a protocol but rather an order that describes what a patient can and cannot have. “Patient may have Free Water Protocol” verses “Patient may have unlimited thin water via cup (no other liquids) between meals starting 30 minutes after meals and after oral care. Patient to be upright for all PO intake.”
The importance of oral care cannot be emphasized enough. Failures with a Free Water Protocol are almost always because the oral care component has not been fully implemented. Oral care in patients with severe dysphagia should be treated as a nursing treatment and may involve the use of oral suction and MD-ordered oral solutions such as chlorhexidine. If nursing has questions about the safest way to administer oral care in these patients, consult the SLP.
The benefits of the Water Protocol include:
- Reducing risk for dehydration and the multiple sequelae from dehydration
- Better adherence to other dietary restrictions
- Decreased re-hospitalizations
If you are interested in implementing a Free Water Protocol and have questions, feel free to reach out to me at ematson@ensignservices.net.





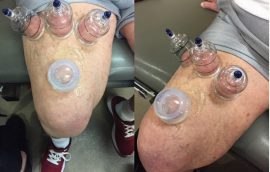 His primary limiting impairments were stiffness, pain and weakness. When he initially attempted basic OKC (open kinetic chain) activities, the patient would report moderate to severe pain at end-range knee extension. The team attempted to modify to a CKC (closed kinetic chain) to assess differences in symptoms. Stiffness remained. Moving to manual therapy, the patient responded decently well with anterior tibiofemoral mobilizations. The patient reported less pain, but the stiffness remained. The PT team applied three hard plastic cups with 1.5 pumps of pressure proximal to the knee as a gross stabilization point for the fascial system and one silicone cup just distal to those cups with the intent to perform a dynamic mobilization technique. Post-treatment, the patient reported that not only was the pain nearly eliminated, but the stiffness was gone as well.
His primary limiting impairments were stiffness, pain and weakness. When he initially attempted basic OKC (open kinetic chain) activities, the patient would report moderate to severe pain at end-range knee extension. The team attempted to modify to a CKC (closed kinetic chain) to assess differences in symptoms. Stiffness remained. Moving to manual therapy, the patient responded decently well with anterior tibiofemoral mobilizations. The patient reported less pain, but the stiffness remained. The PT team applied three hard plastic cups with 1.5 pumps of pressure proximal to the knee as a gross stabilization point for the fascial system and one silicone cup just distal to those cups with the intent to perform a dynamic mobilization technique. Post-treatment, the patient reported that not only was the pain nearly eliminated, but the stiffness was gone as well.

